Dr. Kevin Ko: Your Guide to Tennis Elbow

Lateral epicondylitis, commonly referred to as “tennis elbow”, is one of the most common overuse syndromes, and certainly the most common affecting the elbow. Despite being called tennis elbow, lateral epicondylitis is rarely related to playing tennis, although it absolutely can be.
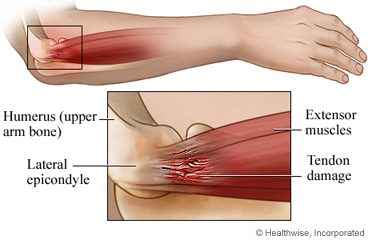
The elbow is comprised of three bones: the humerus (upper arm bone), radius and ulna (the two bones in the forearm). At the distal end of the humerus, closest to the elbow, are two projections for tendon attachment called the epicondyles. There is both a lateral and medial epicondyle. Lateral epicondylitis directly translates to “inflammation of the lateral epicondyle”, and that is our area of focus. The lateral epicondyle serves as the attachment point for many of the muscles that function to extend the wrist.
Repetitive motions and/or heavy lifting put a chronic strain on the tendons that attach to the lateral epicondyle causing micro-tearing and inflammation which can lead to pain and discomfort similar to other common tendonitis-related ailments. Typically, the patient is tender to palpation on the lateral (outside) portion of the elbow right along the extensor tendons and at the lateral epicondyle itself. Symptoms are often aggravated with gripping, wrist supination and pronation (twisting), fine motor activities such as typing, writing, or playing an instrument, and vibratory activities often associated with construction or manual labor. Lateral epicondylitis is typically found in the dominant arm due to heavier use and can last for weeks all the way up to years if left untreated.
There are many treatment options for lateral epicondylitis and they vary from conservative to aggressive.
The first thing to try is the RICE acronym: rest, ice, compression, elevation. When possible, activity avoidance is the surest way to limit the strain being put on the effected tendons. Ice acts as an inflammation suppressant as well as an analgesic. The tendons in this condition are chronically inflamed, so reducing that inflammation can directly result in reducing pain.
Compression through the use of a counterforce brace can be very helpful in alleviating discomfort. The brace is placed just below the elbow and sit of pain and mimics a secondary insertion site for the tendons and can relieve the chronic demand on the actual insertion site.
A wrist brace can also be utilized with the intent of preventing noxious wrist flexion and, specifically, extension. Elevation can be difficult with the upper extremities, but lying flat and lifting the effected arm above the heart can also aid in reducing inflammation.
Non-steroidal anti-inflammatories (NSAIDs) are drugs that can be obtained over-the-counter that decrease inflammation. These drugs can be taken in a pill form and work systemically, or a gel form that works locally where it is applied topically.
Physical therapy is commonly prescribed by the treating provider in conjunction with one of the previously mentioned conservative managements and aims to reduce symptoms by addressing muscle weakness or imbalance, poor body mechanics, and modalities that are very effective at physiologically addressing the injury.
A steroid, or cortisone, injection can be considered if physical therapy and NSAIDs are ineffective. The lateral elbow is injected with a very thin needle and patients often report immediate and significant relief of their symptoms. The relief from an injection typically lasts for up to three months, but can last longer. It is most effective if used in conjunction with physical therapy and other conservative measures. Finally, in persistent cases, if all other treatment options have been exhausted, surgery can be considered and can be very effective at addressing lateral epicondylitis.
Lateral epicondyltis, or tennis elbow, is a very common ailment affecting a wide range of people of all sorts of activity levels, ages, and genders. Recognizing symptoms early is critical to a fast and permanent recovery. If you are wondering if you might be suffering from this condition, please contact OPA and schedule an appointment with Dr. Kevin Ko for consultation and advice.
– Kevin Ko, M.D.
To request an appointment with Dr. Ko, please click here.
Helpful Reading: How Do I Know if My Elbow Injury is Serious