Understanding Abnormal Gait: Causes, Symptoms & How to Fix It
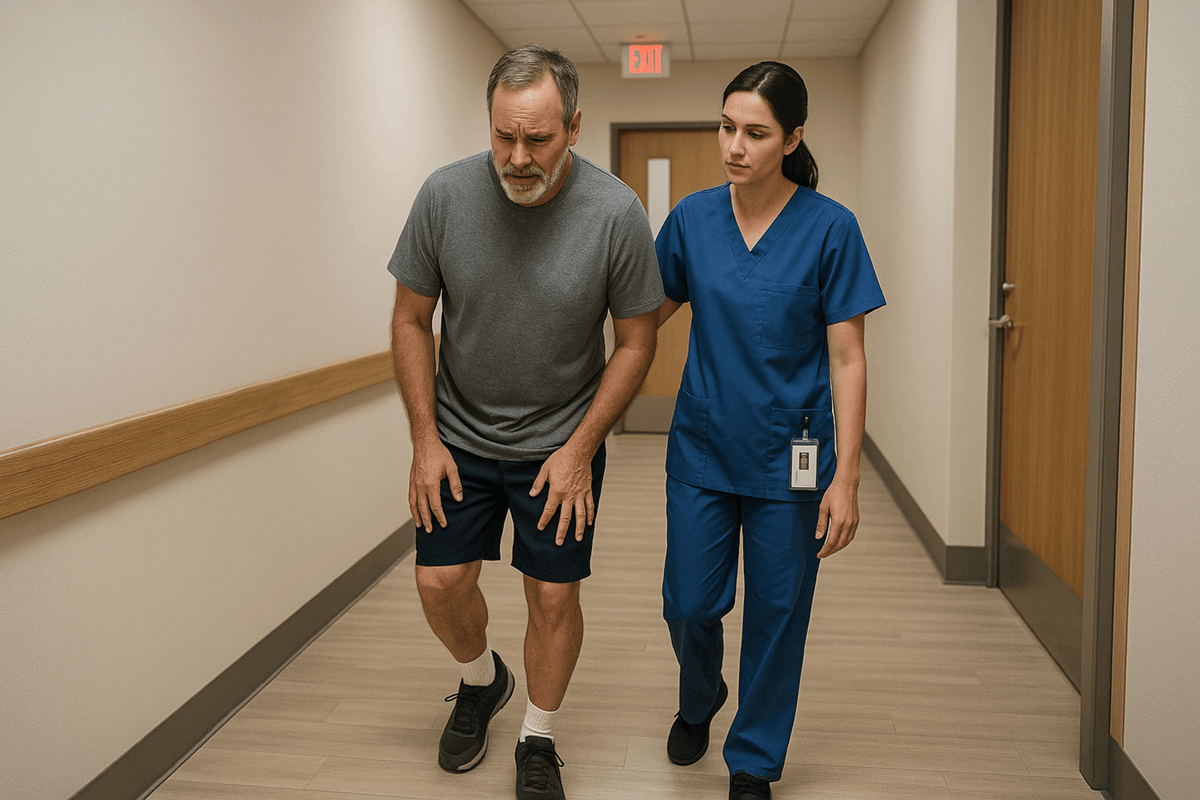
Abnormal gait is a term providers use when your walking pattern changes noticeably. Maybe you’re limping, shuffling, dragging a foot, taking shorter steps, or feeling unsteady.
Sometimes the cause is simple, such as a sore ankle or tight hip flexors. Other times, gait pattern issues can be an early sign of a neurological or musculoskeletal condition that needs medical attention.
This guide explains what is abnormal gait, common abnormal gait symptoms, the types of gait abnormalities, leading abnormal gait causes, how walking problems diagnosis works, and what typically helps at home and in the clinic.
What Is Abnormal Gait?
Your gait is the way you walk: how your feet strike the ground, how your joints move, how your muscles coordinate, and how well you balance. Abnormal gait happens when any part of that system is disrupted by pain, weakness, stiffness, poor coordination, or balance problems from your normal gait.
A brief change after an intense workout or a minor injury can be normal. But if your walking looks or feels different for more than a few days, or it’s getting worse, it’s worth taking seriously. Walking “through it” often trains your body into compensation patterns that can lead to more pain over time.
Common Signs and Abnormal Gait Symptoms
People often notice gait changes before they feel a strong pain signal. Here are common gait imbalance symptoms and warning signs to watch for:
- Limping or favoring one side
- Shuffling gait steps or reduced foot lift (especially when tired)
- Dragging toes or “scuffing” the floor
- Taking shorter steps or walking more slowly than usual
- Feeling unsteady, veering to one side, or needing to hold onto walls/furniture
- Wider stance for stability (“walking like on ice”)
- Difficulty starting, stopping, or turning
- Hip drop or side-to-side sway
- New foot pain, knee pain, hip pain, or back pain when walking
If your symptoms appear suddenly, or you’re also feeling numbness, weakness, severe dizziness, or trouble speaking, seek urgent medical care.
Types of Gait Abnormalities (Common Patterns)
Providers use pattern names to describe types of gait abnormalities. You don’t need to self-diagnose, but understanding the terms can help you describe what you’re experiencing.
Antalgic gait (pain-avoidance limp)
This is one of the most common patterns. You spend less time standing on the painful leg, often stepping quickly off it.
- Common links: arthritis, tendon injuries, sprains/strains, fractures, plantar fasciitis
Spastic gait
This can look stiff or “tight,” sometimes with the leg swinging outward in a semicircle.
- Common links: stroke, multiple sclerosis, spinal cord conditions
Ataxic gait
Often wide-based and unsteady, with a swaying feeling, especially when turning.
- Common links: balance/inner ear issues, cerebellar conditions, medication effects
Parkinsonian gait
Typically shuffling with smaller steps, reduced arm swing, and difficulty initiating movement (“freezing”).
- Common links: Parkinson’s disease and related disorders
Steppage gait (often related to foot drop)
You may lift your knee higher to clear the toes, and the foot may slap down.
- Common links: nerve compression, peripheral neuropathy, lumbar radiculopathy
Waddling gait / Trendelenburg-type gait
This can look like side-to-side sway or a hip “drop,” often due to hip muscle weakness.
- Common links: hip abductor weakness, hip arthritis, muscle conditions
These are examples of gait disorders explained in practical terms: the pattern is a clue that helps a clinician narrow down the cause.
Abnormal Gait Causes: Why Walking Changes
There are many abnormal gait causes, but most fall into a few main categories.
Musculoskeletal Causes
These are very common and usually involve pain, stiffness, or weakness in joints and soft tissues.
- Hip, knee, ankle, or foot arthritis
- Tendonitis or tendon tears (Achilles, gluteal tendons, etc.)
- Ligament sprains and instability (ankle/knee)
- Muscle strains or significant tightness
- Leg-length differences
- Foot structure issues (high arches, flat feet) affecting mechanics
Neurological Causes
Neurological conditions can affect coordination, muscle control, sensation, and balance.
- Stroke, Parkinson’s disease, multiple sclerosis
- Peripheral neuropathy (often associated with diabetes)
- Nerve compression in the spine or leg (sciatica/radiculopathy)
- Conditions affecting the inner ear or balance systems
Injury-related Causes
Walking changes are common after injuries—even when the injury “seems healed.”
- Fractures, post-surgical stiffness, scar tissue
- Compensation after a sprain or meniscus injury
- Pain-related guarding patterns that become habits
Systemic and other contributors
Some health issues affect energy, strength, sensation, or stability.
- Medication side effects (sedating, dizziness, movement changes)
- Deconditioning after illness or inactivity
- Vision changes affecting balance and confidence
In short, the causes of walking abnormalities can be local (foot/ankle pain) or system-wide (nerve or balance issues).
Risk Factors and When to See a Doctor
You should consider a medical evaluation to diagnose gait abnormalities if:
- Your gait change lasts more than 1–2 weeks
- You’re experiencing repeated stumbles or falls
- Pain is increasing or spreading to the back/other joints
- You notice new weakness, numbness, or foot drop
- Your walking is limiting work, exercise, or daily activities
Seek urgent care if gait changes are sudden and paired with stroke-like symptoms (facial droop, weakness on one side, slurred speech), severe dizziness, or an inability to walk.
Walking Problems Diagnosis: How Abnormal Gait Is Evaluated
A good walking problems diagnosis usually includes:
Medical history and physical exam
Your provider will ask when it began, what worsens it, and where you feel pain. They’ll check joint range of motion, strength, alignment, and tenderness.
Gait analysis (basic or advanced)
This can be as simple as observing you walk, turn, and balance, or a more detailed video analysis in a rehab setting. The goal is to identify the specific gait pattern issues driving symptoms.
Neurological exam (when indicated)
Your provider may test reflexes, sensation, coordination, and muscle tone, especially if balance changes, numbness, or weakness are present, to diagnose neuropathic gait.
Imaging and tests (as needed)
X-rays can evaluate bone alignment and arthritis. MRI may be used for soft tissue or spine concerns. In some cases, labs may help rule out systemic contributors.
Gait Disorder Treatment Options (How to Fix It)
The right gait disorder treatment depends on the cause, but many plans include a combination of these approaches:
Physical therapy and gait retraining
PT is often the foundation of treatment because it addresses strength, flexibility, balance, and movement habits, not just symptoms.
- Hip/core strengthening for stability
- Ankle mobility and calf strength for push-off
- Balance work to reduce fall risk
- Step mechanics and cadence training to improve symmetry
Orthotics, braces, and footwear changes
Supportive shoes, custom inserts, or braces can improve mechanics and reduce pain, especially for feet/ankles and certain knee/hip issues.
- Examples: arch support orthotics, ankle braces, AFO for foot drop
Medications and injections (when appropriate)
Anti-inflammatory strategies can help with pain-driven limping. Some neurological conditions require targeted medications managed by a specialist.
Procedures or Surgery (when necessary)
If conservative care fails or there’s significant structural damage, surgery may be recommended (for example, advanced arthritis or certain tendon/ligament injuries).
Home Exercises & Gait Correction Tips
If your symptoms are mild and you don’t have red flags, these gentle steps can help. Stop if pain is sharp, worsening, or accompanied by numbness/weakness.
- Shorten your stride for a few days to reduce stress while healing
- Use supportive footwear (avoid worn-out shoes or slippery soles)
- Calf stretch + ankle pumps to improve ankle motion
- Heel raises (holding a counter) to build calf strength
- Clamshells or side-lying hip abduction to strengthen hip stabilizers
- Supported balance practice (tandem stance or single-leg stand near a wall)
If you’re limping, it’s a sign your body is protecting something. If it persists, don’t “push through”; get evaluated.
Complications If Left Untreated
Untreated abnormal gait can lead to:
- Higher fall risk and injury risk
- Worsening joint overload (hip, knee, back, joint pain)
- Reduced mobility and endurance
- Chronic compensation patterns that are harder to correct later
Prevention & Long-Term Management
The best long-term strategy is simple and consistent:
- Maintain hip, core, and ankle strength
- Address injuries early and complete rehab (even if pain improves)
- Manage chronic conditions (like diabetes or arthritis) with your care team
- Get vision and balance concerns checked
- Reassess footwear and walking habits regularly
The Bottom Line
Abnormal gait is more than “walking funny.” It’s your body’s way of signaling pain, weakness, balance problems, or coordination changes.
By recognizing early abnormal gait symptoms, understanding the major types of gait abnormalities, and getting a proper walking problems diagnosis, you can choose the right gait disorder treatment, from physical therapy and orthotics to medical management when needed.
If your gait change is persistent, painful, or affecting balance, an orthopedic or sports medicine evaluation can help pinpoint the cause and build a clear plan to get you walking confidently again. Contact OPA Ortho to schedule a professional evaluation and take the first step toward safer, stronger movement.

